Disability Determination Decision Under Review Step 2 of 3
Bernard Wixon is with the Function of Policy Evaluation and Modeling, Role of Enquiry, Evaluation, and Statistics (ORES), Office of Retirement and Disability Policy (ORDP), Social Security Administration (SSA). Alexander Strand is with the Office of Economic Analysis and Comparative Studies, ORES, ORDP, SSA.
Acknowledgments: For helpful information or comments, we thank the following: Bob Appleton, Clark Burdick, Joan Burke, Sherry Dodson, Eli Donkar, Steve Duffy, Jim Fahlfedder, Terrance Flannery, Susan Grad, Nitin Jagdish, Sharon R. Johnson, Kathy Mahan, David Pattison, Clark Pickett, Mary Quatroche, Joshua Silverman, Jim Twist, and Tim Zayatz.
The findings and conclusions presented in this note are those of the authors and practice non necessarily stand for the views of the Social Security Administration.
Introduction
| DDS | Disability Determination Service |
| DI | Disability Insurance |
| NDDSS | National Disability Determination Services Organization |
| RBC | Regulation Basis Code |
| SGA | substantial gainful activity |
| SSA | Social Security Administration |
| SSI | Supplemental Security Income |
Under the disability determination process used by the Social Security Administration (SSA), each determination that an applicant is either eligible (allowed) or ineligible (denied)—nether Disability Insurance (DI) and/or Supplemental Security Income (SSI)—has a specific regulatory basis that is cited by program administrators. Decomposing broad inability trends requires identification of those bases and the steps of the determination procedure at which they are cited. For case, the contempo increase in the number of allowances has been accompanied past a modify in the composition of allowances. For DI, the percentage of allowances based on vocational, educational, and historic period-specific factors increased from 28 percent to 47 percent in the 10 years prior to 2009 (SSA 2011a). In this case, decomposing recent programme growth permits researchers to place subcategories driving the growth. To give another case, decomposing trends in denials at various steps of the determination process may permit researchers to consider to what extent the process counterbalances increases in applications during recessions, keeping program costs in check.
The purpose of this note is to facilitate research on trends in allowances and denials by documenting how the steps of the determination process and the bases for medical eligibility decisions tin be identified in authoritative data. Specifically, the steps in the initial determination process tin be identified using the Regulation Ground Code (RBC), which appears in Social Security's authoritative data systems as well as related research information sets. The RBC documents the detailed reason for each SSA determination, in terms of medical, medical-vocational,i and other criteria. The RBC is recorded in the National Inability Determination Service Organisation (NDDSS); in turn, the NDDSS is used to construct the so-called 831 disability applicant files (from Form SSA-831 data) too every bit related inquiry files. We classify the RBCs by programme and age (DI, SSI adult, SSI child) and pace of the decision process at which they are invoked. Our frequency tabulations evidence that some codes are numerically important at a given step and others correspond a range of technical denials, rare findings, or data errors. Further, we provide the proportions of determinations observed for each ground code at each step, using the 831 file for 2010 equally a benchmark.
Program Background
The two disability programs administered past SSA have fiscal and nonfinancial criteria for eligibility. In the instance of the DI plan, financial eligibility is based on (1) past earnings criteria involving the total number of quarters worked while making Federal Insurance Contributions Deed (FICA) contributions, and (ii) the number of quarters worked in years immediately before disability onset. Both criteria are used to define the bidder's insured status. For SSI, fiscal eligibility is based on current income and resource2 to target payments to individuals with limited financial means.
While the nonfinancial benchmark for SSA's retirement program is straightforward (if the applicant's age is greater than or equal to the total retirement age or the early on retirement age, then the bidder is eligible), the nonfinancial (largely medical) criteria for DI benefits (or for SSI disability payments) are complex. In fact, at that place are multiple medical criteria—or combinations of medical and vocational criteria—under which an bidder tin exist constitute medically eligible or medically ineligible. In addition, there are outcomes that are not medical in nature; for example, an applicant can exist denied if he or she refuses to submit to a consultative examination or refuses to follow prescribed treatment.
SSA uses the aforementioned disability conclusion procedure in administering the two disability programs, DI and SSI. Financial and other nonmedical screens are implemented by SSA field offices. For applicants plant eligible under those screens, the initial medical determinations are fabricated past Disability Determination Service (DDS) agencies in each land. However, if an applicant is denied at the initial DDS level, he or she has the option of pursuing a sequence of appeals, including highly-seasoned to (1) the DDS itself, known every bit afterthought;3 (2) an administrative constabulary guess (ALJ); (three) the Appeals Council; and finally (iv) a federal courtroom.
The RBC records data almost the determinations fabricated past the DDS, including initial determinations and reconsiderations. The purpose of this note is to help researchers and program analysts translate the particular medical, medical/vocational, or other criterion that is invoked by the DDS in its allow/deny determination of a given applicant. The importance of the RBC is that it permits an analyst to parse plan outcomes in terms of the effects of the particular medical, medical/vocational, or other criterion used to make up one's mind medical eligibility. Adjacent, we outline the sequential inability determination process used by SSA and DDS agencies—the conclusion-making structure underlying field part intake decisions and the detailed DDS determination outcomes represented in the RBC.
SSA's Disability Conclusion Process
The disability conclusion procedure described in this study is used by Social Security field offices and state DDS agencies to make initial disability determinations. Field offices implement step 1 of the five-step disability conclusion procedure, and DDS agencies are responsible for the medical determinations at stepstwo–5. The specific criteria used by the DDS in its allow/deny determinations are identified in the RBC, which is included in the NDDSS data generated by DDS agencies. The RBC describes the basis for initial determinations and reconsiderations. Outcomes of college-level appeals, such every bit decisions of ALJs, are in principle, based on the same criteria as DDS determinations, but such appeals decisions are not included in the NDDSS information generated by DDS agencies. ALJ-level decisions are recorded in the Case Processing and Direction System.
Sometime Commissioner Robert Grand. Ball (1978) provides an insight that is useful in trying to understand the design of the determination process. For the sake of efficiency, the process implies a screening strategy:
The thought was to screen quickly the large majority of cases that could exist allowed on reasonably objective medical tests and so deal individually with the troublesome cases that didn't pass the screen. (157)
For example, the showtime three stages of the adult disability conclusion procedure correspond screens:
- claimants who are engaging in substantial gainful activity (SGA) are denied (pace i) without any consideration of medical criteria,
- those without severe impairments are denied (step ii), and
- those with the most highly disabling or fatal impairments are immune (step 3).
In Ball's characterization, the "troublesome" cases are the rest, which are evaluated on a case-by-case ground using both medical and vocational factors (stride 4 and possibly footstep 5).4
Because the processes for adults and children differ, we discuss them separately.
Adults
The steps in the inability determination process for adults are diagrammed in Chart i, adapted from Lahiri, Vaughan, and Wixon (1995).
Chart 1.
Disability determination for adults
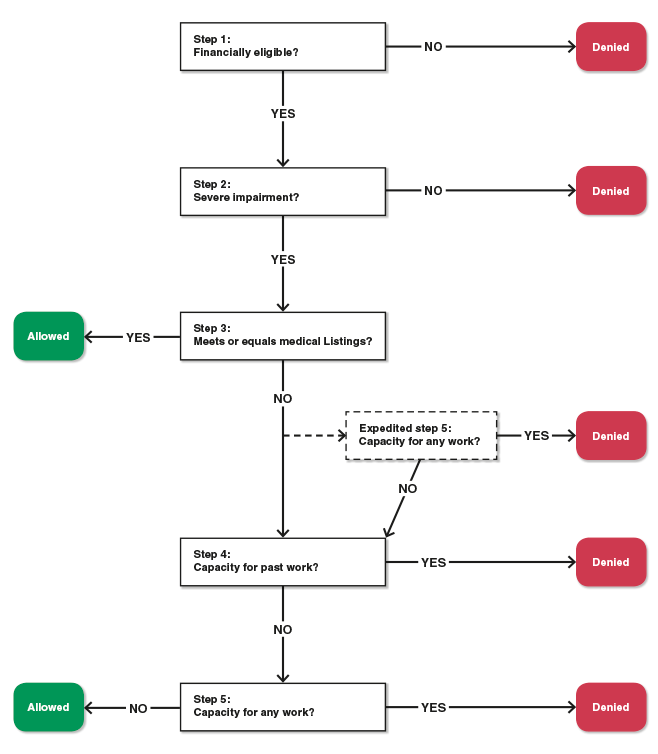
SOURCE: Authors' illustration adjusted from Lahiri, Vaughan, and Wixon (1995).
Step ane: Financial screens. For both DI and SSI, Social Security field offices screen out applicants who work and have earned income above the SGA limit. Those claims are denied on the basis of applicants' work action. SGA is "work that involves doing significant and productive concrete or mental duties and is washed (or intended) for pay or profit."5 In most cases, applicants with earnings above the SGA threshold corporeality are denied on grounds that their earnings indicate that they are not permanently and totally work disabled; otherwise, the application is referred to the DDS.6 The SGA amount for nonblind beneficiaries was $1,010 per month in 2012.
In add-on, field offices verify insured status for DI applicants. Analogously, field offices ensure that countable income and resources are below the relevant thresholds for SSI applicants. These financial determinations are not technically part of the sequential decision process and thus are not represented in the RBC, but for the sake of efficiency, they are normally undertaken (at least on a preliminary basis) past field offices as part of the step i process.vii
Step 2: A medical screen to deny applicants without a astringent impairment. An applicant is denied at footstep ii if his or her impairment(s) is considered non severe. According to SSA'southward Program Operations Manual Organisation (POMS), under step two:
"information technology must be determined whether medical testify establishes a concrete or mental harm or combination of impairments of sufficient severity as to exist the basis of a finding of inability to engage in any substantial gainful activity (SGA). When medical evidence establishes only a slight abnormality or a combination of slight abnormalities which would have no more than a minimum effect on an individual'south ability to work, such damage(south) will be plant "not severe," and a determination of "not disabled" volition be made…"8
Applicants are likewise denied if their impairments neglect the elapsing test; that is, if the harm (1) is not expected to consequence in death, and (2) has neither lasted 12 months nor is expected to last for a continuous period of 12 months. The elapsing test is typically invoked at step ii, simply may also be invoked at step 3, 4, or 5.
Stride 3: A medical screen to allow applicants who are the virtually severely disabled. Medical evidence on an applicant'due south impairment is assessed under step 3 using codification clinical criteria called the List of Impairments, which includes over 100 impairments. Applicants with impairments that "run into" the Listings are immune with no further evaluation, based solely on medical criteria. Moreover, if an applicant has an harm not included in the Listings, only considered medically equivalent to a listed impairment, the impairment is said to "equal the Listings" and the applicant is immune.nine Applicants who are non allowed at step 3 accept impairments that, although severe, are not severe plenty to consider the applicants disabled purely on medical grounds. Such applicants are evaluated further at step 4 and, possibly, pace 5.
Footstep four: Can severely impaired applicants piece of work in their by jobs? At this step, the DDS considers whether an applicant's residual functional capacity (RFC) meets the skill and task requirements of his or her past relevant work. The evaluation of RFC determines to what extent the bidder can perform basic work-related activities associated with jobs previously held—unremarkably jobs held in the 15 years before adjudication.x Applicants who are judged able to perform past work are denied; the claims of remaining applicants are passed on for evaluation under step 5.
Step 5: Can severely impaired applicants exercise other piece of work in the national economy? At pace 5, the applicant's RFC is considered, along with vocational factors—specifically, age, education, and work experience—to determine whether he or she tin piece of work in jobs other than those previously held. The vocational factors are used to decide whether the applicant can work in employment consistent with his or her residue capacity. This determination often involves the use of a set up of tables referred to equally the medical-vocational guidelines (sometimes known as the vocational grid 11) and medical vocational profiles.12 At step 5, remaining applicants are either immune or denied.
Beginning in 1999, SSA implemented modifications to the disability determination procedures in states known as prototype states.13 Ane modification was to permit DDS decision makers the discretion to proceed directly to step 5 when there is insufficient prove about the claimant's work history to brand the evaluation at step four. Nether this procedure, referred to as expedited vocational assessment, applicants may be denied if they are judged able to perform work in the national economy. However, if they are judged unable to do that, the DDS is required to return to and consummate footstep 4. Expedited vocational cess was extended to the other states in August 2012.14
SSI Children
Some of the steps in the disability decision process for children are similar to those for adults. Steps in the process for children are diagrammed in Chart two.
Chart two.
Inability determination procedure for children
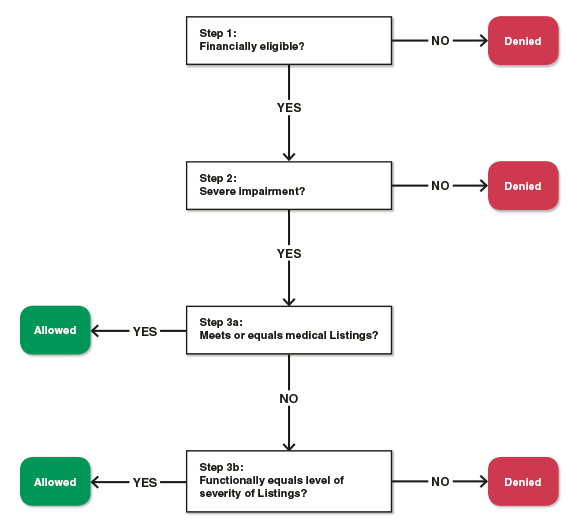
SOURCE: Authors' illustration.
Notation: Although the disability determination procedure for children includes a medical screen and a functional assessment as a unmarried step (step three), for analytical purposes we discuss them separately as step 3a and footstep 3b.
Stride i: Financial screens. Children may not qualify for DI benefits on their own earnings record.xv Still, they may qualify for SSI payments on their own in some cases or as part of a unit including their parent(s). For SSI, field offices evaluate income and resource eligibility nether a complex prepare of rules. Field offices also verify whether the kid is working at SGA because those upwardly to age 18, some of whom may be working, are evaluated nether the determination procedure for children. If a child is engaging in SGA, the merits is denied and not referred to the DDS.
Step 2: A medical screen to deny applicants without a severe impairment. The DDS denies a child bidder at step 2 if he or she does not have a medically determinable harm or if his or her impairment(due south) is considered not severe. Child applicants are also denied if their impairments fail the duration test; that is, if the impairment (1) is non expected to result in death, and (2) has neither lasted 12 months nor is expected to final for a continuous flow of 12 months. If the damage(s) is considered severe and if whatsoever harm meets the duration test, the merits volition proceed to the next step.
Step 3a:16 A medical screen to allow the well-nigh severely impaired applicants. If the child has ane or more than severe impairments, the DDS will determine if any astringent impairment meets one of the Listings for children. The Listings encompass the major body systems and include descriptions of common physical and mental impairments (such as cerebral palsy, mental disorders, and asthma), along with specific medical severity criteria. As with adults, if the impairment does not meet the Listings, the DDS decides if information technology medically equals the Listings. If the child has ane or more than impairments that meet or medically equal the requirement of a List and meet the duration requirement, the DDS volition discover the child disabled and the determination is consummate.
Step 3b: Can a severely impaired child office at abode, at schoolhouse, and in the community? If the child has one or more than impairments that are severe but practise non meet or medically equal a List, the DDS will decide whether the impairment or impairments "functionally equal" the Listings. That means that the DDS assesses the furnishings of whatever impairment on the child'south ability to part at abode, at school, and in the customs. In particular, the DDS considers questions such as—
- What activities is the child able or not able to perform?
- Which activities are express in comparing with children of the aforementioned age without the harm?
- What type and corporeality of help does the kid need to complete age-advisable activities?
Once the DDS has evaluated the extent to which the child can perform activities, it evaluates how much the kid is limited in each of six domains. The domains are broad areas of operation intended to capture all that a kid tin or cannot practise. The six domains are as follows:
- Acquiring and using data,
- Attending to and completing tasks,
- Interacting and relating with others,
- Moving almost and manipulating objects,
- Caring for himself or herself, and
- Maintaining health and concrete well-being.
If a child's impairment or combination of impairments results in "marked" limitations in two or more of these domains of operation, or an "farthermost" limitation in i domain, and then his or her impairment(s) functionally equals the Listings. A marked limitation in a domain is one in which a child's impairment interferes seriously with his or her ability to independently initiate, sustain, or consummate activities. An extreme limitation in a domain is one in which a child'south harm interferes very seriously with those abilities.
Identifying the Sequential Steps Using Regulation Footing Codes
The detailed RBC values are somewhat different for DI (under ChampionshipII—Sometime-Age, Survivors, and Disability Insurance—of the Social Security Deed) and SSI (under TitleXVI of the Act) and, because they include a number of administrative outcomes, are considerably more detailed than the sequential conclusion steps might propose.
We recode the individual regulation footing values into sequential inability determination steps in Tables i through 3. In deriving the recode, we consulted program experts and the documentation from Social Security authoritative sources—the footing for mean solar day-to-day use of RBCs by plan administrators. We besides compared coding from other sources by examining the coding that is used in almanac SSA publications. Specifically, the Annual Statistical Report on the Social Security Disability Insurance Program (SSA 2011a, Tables 63 and 64) classifies medical decisions at step 2 onward for DI determinations. The SSI Almanac Statistical Report (SSA 2011b, Tables 73 and 74) does a like nomenclature for SSI determinations. In addition, nosotros prepared the coding that was used in several analytical studies, including Lahiri, Vaughan, and Wixon (1995); Hu and others (2001); Dwyer and others (2002/2003); Lahiri, Song, and Wixon (2008); and Autor and others (2011). We also compared those different coding schemes and consolidated differences.17 These comparisons establish the broad consistency of the recode presented here with documentation from plan administrators, published tables, and recent analyses.
The frequencies of the sequential disability determination steps are shown in Tables one through 3 using the 831 file for 2010.18 When comparing those results to frequencies based on other data sources, several features of the sample universe used in our tabulations should exist noted. First, data are shown for chief DI and SSI disability claims, where the claimant is a worker (for DI claims), an SSI adult, or an SSI kid. Second, step 1 determinations are generally not included because the majority of those decisions are made in the field offices. Denials made at the field function level are not referred to the DDS and are not represented in the NDDSS data. Third, researchers often remove 831 observations that can functionally be considered duplicates. For example, because the 831 information are transaction based, if an applicant filed more than than one claim for the same program, each merits would generate a new tape. Moreover, if the researcher is undertaking a person-based assay, he or she may choose to purge records then that each person is represented by a single tape. We show frequencies with duplicates included equally a benchmark that could be hands replicated. Finally, our frequency tabulations include only DDS initial determinations; that is, for DDS denials that are appealed, our tabulations do not represent the final decision made by SSA.
In this notation, we draw the steps in the initial inability determination process and provide a classification of RBCs for DDS decisions made in 2010.19 This will allow researchers to create classifications that are comparable to official SSA publications and previous analytical studies. We hope this facilitates inquiry about trends in disability claims and the outcomes of those claims.
| Code | Decision | Ground | Number | Per centum |
|---|---|---|---|---|
| Footstep 1: Engaging in SGA?a | 165 | 0.0 | ||
| N1 | Deny | Engaging in SGAb—ER/PP metc | 152 | 0.0 |
| N2 | Deny | Engaging in SGA—ER/PP not met | thirteen | 0.0 |
| Step 2: Severe impairment? | 384,175 | 15.8 | ||
| Severity | ||||
| F1 | Deny | Damage not severe—ER/PP/reentitlement period met | 115,287 | 4.seven |
| F2 | Deny | Impairment not severe—ER/PP/reentitlement period non met | 185,324 | seven.6 |
| Durationd | ||||
| E1 | Deny | Harm prevented SGA < 12 months—ER/PP/reentitlement period met | 2,796 | 0.1 |
| E2 | Deny | Harm prevented SGA < 12 months—ER/PP/reentitlement period non met | 453 | 0.0 |
| E3 | Deny | Impairment not expected to last 12 months—ER/PP/reentitlement period met | 78,184 | iii.2 |
| E4 | Deny | Impairment non expected to last 12 months—ER/PP/reentitlement period not met | ii,131 | 0.1 |
| Step three: Meets or equals the Listings? | 330,383 | xiii.6 | ||
| A1 | Allow | Damage meets the Listings | 271,278 | 11.1 |
| B1 | Allow | Impairment equals the Listings | 59,105 | 2.iv |
| Stride 4: Capacity for past work? | 499,238 | 20.v | ||
| H1 | Deny | Capacity for SGA, past relevant work—ER/PP met | 448,993 | xviii.4 |
| H2 | Deny | Chapters for SGA, past relevant work—ER/PP not met | 50,245 | 2.one |
| Stride 5: Capacity for any work? | 1,042,622 | 42.8 | ||
| C1 | Allow | Medical vocational considerations | 408,301 | 16.viii |
| D1 | Allow | Medical vocational considerations—arduous unskilled work | 310 | 0.0 |
| G1 | Deny | Capacity for SGA, vocational considerations—reentitlement period met | 34,131 | 1.4 |
| G2 | Deny | Capacity for SGA, vocational considerations—reentitlement period not met | 1,225 | 0.ane |
| J1 | Deny | Capacity for SGA, other piece of work—ER/PP met | 529,680 | 21.seven |
| J2 | Deny | Chapters for SGA, other work—ER/PP not met | 68,975 | 2.viii |
| Other | 180,961 | 7.iv | ||
| CE | Allow | Collateral estoppeleast | 7,141 | 0.iii |
| K1 | Deny | Failure to follow prescribed handling—ER/PP/reentitlement period met | 161 | 0.0 |
| K2 | Deny | Failure to follow prescribed treatment—ER/PP/reentitlement menses not met | 42 | 0.0 |
| L1 | Deny | Failure/refusal to submit to CE—ER/PP/reentitlement period met | 57,612 | 2.4 |
| L2 | Deny | Failure/refusal to submit to CE—ER/PP/reentitlement period not met | 5,470 | 0.2 |
| M3 | Deny | Does not want to go along claim development; use evidence in file— ER/PP/reentitlement period met | 5,522 | 0.2 |
| M4 | Deny | Does not want to continue claim development; use evidence in file— ER/PP/reentitlement menstruum non met | 473 | 0.0 |
| M5 | Deny | Bereft bear witness—ER/PP/reentitlement menstruation met | 74,711 | 3.ane |
| M6 | Deny | Insufficient evidence—ER/PP/reentitlement menses not met | 21,885 | 0.9 |
| M7 | Deny | Does not want to continue merits evolution; practise not apply evidence in file— ER/PP/reentitlement menses met | 826 | 0.0 |
| M8 | Deny | Does not want to continue merits development; do not use evidence in file— ER/PP/reentitlement flow not met | 100 | 0.0 |
| S1 | Deny | Res judicataf—ER/PP not met | 2,191 | 0.1 |
| X3 | Deny | Medicare butg—AOD on or after age 62 years and 7 months/or not disabled, whereabouts unknown | ix | 0.0 |
| Z1 | Deny | DAAh is fabric to the determination of inability—ER/PP/reentitlement flow met | 3,839 | 0.two |
| Z2 | Deny | DAA is material to decision of inability—ER/PP/reentitlement flow not met | 968 | 0.0 |
| ZZ | Regulation Basis Code is unknown | 2 | 0.0 | |
| [blank] | Regulation Footing Code is non available | ix | 0.0 | |
| Total | ii,437,544 | 100.0 | ||
| SOURCES: Frequency data was obtained from the 2010 SSA-831 file. Basis information was obtained from RAND's SSA Plan Data User's Manual (Panis and others 2000) and exchanges with disability experts at SSA. | ||||
| NOTES: Values may not sum to 100 because of rounding. AOD = declared onset date; | ||||
| a. Fiscal eligibility for DI or SSI is commonly determined at the SSA field office before the merits is referred to the DDS. For that reason, nigh cases determined financially ineligible are not referred to the DDS and are non represented in the 831 data created by the DDS. Nevertheless, in a few cases, claims referred to the DDS tin be sent back to the field office or recalled by the field office; such cases may be found in the 831 data. Some cases may besides exist for applicants alleging blindness, but the college bullheaded SGA cannot be used until the DDS establishes incomprehension. | ||||
| b. SGA is an earnings threshold used to decide eligibility for both DI benefits and SSI payments. In calendar year 2012, the SGA threshold was $1,010 per calendar month for the nonblind and $1,690 for the bullheaded. Someone engaging in SGA is denied at the field office and not evaluated further. And, a DI beneficiary receives no benefits for whatsoever month in which he or she has earnings above the SGA threshold (with some exceptions for work incentives). The SGA threshold is wage-indexed. | ||||
| c. ER/PP/reentitlement period met (or not met): Based on the 1999 Ticket to Piece of work Legislation, Ticket to Work clients who take fabricated a piece of work try but are unable to work considering of their impairments may be eligible for ER to benefit condition. ER applicants receive temporary benefits for a PP, until a medical evaluation of their reinstatement request is completed. | ||||
| d. Duration denials are typically made at pace 2, only may likewise be made at steps 3, iv, or 5. The elapsing test does not utilise to the statutorily bullheaded, aged 55 or older. | ||||
| e. Collateral estoppel: If at that place has been a prior favorable determination past SSA or the court, information technology must be adopted for the aforementioned flow on the new claim, with certain exceptions. | ||||
| f. Res judicata (deprival): The finding for a prior denial is adopted under two assumptions: (1) that the relevant facts about an applicant's disability have not changed and (2) that the criteria under which the before conclusion was made take non become less restrictive. | ||||
| k. Medicare-only instance: Federal workers ineligible for DI, simply eligible for Medicare. | ||||
| h. Prior to 1996, DI beneficiaries and SSI recipients could receive benefits based on an impairment associated with DAA, provided they fulfilled handling requirements. Subsequently passage of Public Law104-121 in 1996, such benefits were ended although some beneficiaries continued to receive benefits based on impairments not associated with DAA. | ||||
| Code | Decision | Basis | Number | Percent |
|---|---|---|---|---|
| Stride 1: Engaging in SGA?a | 0 | 0.0 | ||
| 33 | Deny | Engaging in SGAb | 0 | 0.0 |
| Step 2: Severe impairment? | 215,282 | 10.one | ||
| Severity | ||||
| 30 | Deny | Damage not astringent—no visual allegationc | 139,524 | half-dozen.half-dozen |
| 41 | Deny | Impairment non severe—visual accusation | half-dozen,999 | 0.iii |
| Durationd | ||||
| 34 | Deny | Damage prevented SGA < 12 months—no visual allegation | ii,315 | 0.i |
| 35 | Deny | Impairment not expected to last 12 months—no visual accusation | 65,082 | iii.1 |
| 45 | Deny | Impairment prevented SGA < 12 months—visual allegation | 97 | 0.0 |
| 46 | Deny | Impairment not expected to last 12 months—visual allegation | 1,265 | 0.1 |
| Step 3: Meets or equals the Listings? | 261,750 | 12.3 | ||
| 61 | Allow | Impairment meets the Listings | 220,310 | x.3 |
| 62 | Allow | Impairment equals the Listings | 41,440 | one.9 |
| Pace 4: Chapters for by piece of work? | 402,416 | xviii.nine | ||
| 31 | Deny | Chapters for SGA, past relevant work—no visual allegation | 386,411 | eighteen.2 |
| 42 | Deny | Chapters for SGA, past relevant work—visual accusation | 16,005 | 0.viii |
| Step 5: Capacity for any piece of work? | 993,844 | 46.7 | ||
| 63 | Allow | Medical vocational considerations | 271,022 | 12.vii |
| 64 | Allow | Medical vocational considerations—backbreaking unskilled work | i,080 | 0.1 |
| 32 | Deny | Capacity for SGA, other piece of work—no visual allegation | 690,181 | 32.iv |
| 43 | Deny | Capacity for SGA, other work—visual allegatione | 31,561 | i.5 |
| Other | 255,560 | 12.0 | ||
| CE | Allow | Collateral estoppelf | 356 | 0.0 |
| 36 | Deny | Insufficient evidence—with/without visual allegation | 123,799 | v.8 |
| 37 | Deny | Failure/refusal to submit to CE—with/without visual allegation | 116,635 | v.five |
| 38 | Deny | Does not want to go along development of claim—with/without visual allegation | 4,768 | 0.2 |
| 39 | Deny | DAA or failure to follow prescribed handling—with/without visual allegationg | seven,104 | 0.3 |
| Data errorsh | 2,898 | 0.1 | ||
| Full | 2,128,852 | 100.0 | ||
| SOURCES: Frequency information was obtained from the 2010 SSA-831 file. Basis information was obtained from RAND'southward SSA Program Information User's Manual (Panis and others 2000) and exchanges with disability experts at SSA. | ||||
| NOTES: CE = consultative exam; CE is likewise a Regulation Ground Code; | ||||
| a. Financial eligibility for DI or SSI is normally determined at the SSA field office before the claim is referred to the DDS. For that reason, near cases determined financially ineligible are non represented in the 831 data created by the DDS. | ||||
| b. SGA is an earnings threshold used to make up one's mind eligibility for both DI benefits and SSI payments. In calendar year 2012, the SGA threshold was $1,010 per month for the nonblind and $1,690 for the blind. Someone engaging in SGA is denied at the field office and not evaluated farther. And, a DI casher receives no benefits for any month in which he or she has earnings above the SGA threshold (with some exceptions for work incentives). The SGA threshold is wage-indexed. | ||||
| c. No visual allegation means the bidder does not have a visual impairment that requires a determination under statutory criteria for blindness. | ||||
| d. Duration denials are typically made at stride ii, just may also be fabricated at steps iii, iv, or five. The elapsing test does not apply to SSI applicants who are statutorily blind. | ||||
| due east. Lawmaking 43 has dual meanings. For child applicants it indicates that the claim is denied at step iii considering it neither meets, nor equals, nor functionally equals the Listings. | ||||
| f. Collateral estoppel: If there has been a prior favorable determination past SSA or the court, information technology must be adopted for the same menses on the new claim, with sure exceptions. | ||||
| grand. Code 39 has the aforementioned meaning and utilize for adult and kid SSI applicants. Information technology signifies denial for failure to follow prescribed treatment or, following a 1996 Congressional Act, denial of applicants for whom DAA was establish material to the finding of disability. | ||||
| h. Includes records with unknown RB (RBC = ZZ), RB non bachelor (RBC = [bare]), obsolete codes, and other data errors. | ||||
| Code | Decision | Ground | Number | Percent |
|---|---|---|---|---|
| Stride 1: Engaging in SGA?a | 0 | 0.0 | ||
| 33 | Deny | Engaging in SGAb—with/without visual allegationc | 0 | 0.0 |
| Pace 2: Severe harm? | 34,030 | 6.iv | ||
| Severity | ||||
| 44d | Deny | Impairment not severe—with/without visual allegation | 31,527 | v.ix |
| Duratione | ||||
| 34 | Deny | Harm prevented SGA < 12 months—no visual allegation | 317 | 0.1 |
| 35 | Deny | Damage not expected to last 12 months—no visual allegation | ii,071 | 0.4 |
| 45 | Deny | Harm prevented SGA < 12 months—visual allegation | 37 | 0.0 |
| 46 | Deny | Impairment not expected to last 12 months—visual accusation | 78 | 0.0 |
| Step 3a:f Meets or equals the Listings? | 87,683 | 16.v | ||
| 61 | Allow | Damage meets the Listings | 75,466 | 14.2 |
| 65 | Allow | Medically equals the Listings | 12,217 | 2.3 |
| Step 3b: Functionally equals severity of the Listings? | 379,298 | 71.v | ||
| 66 | Allow | Harm functionally equals the Listing requirements | 109,849 | 20.7 |
| 43 | Deny | Neither meets, nor medically equals, nor functionally equals the Listingsg | 269,449 | 50.8 |
| Other | 29,167 | 5.5 | ||
| CE | Allow | Collateral estoppelh | 21 | 0.0 |
| 36 | Deny | Insufficient show—with/without visual allegation | ten,440 | ii.0 |
| 37 | Deny | Failure/refusal to submit to CE—with/without visual accusation | 14,710 | two.8 |
| 38 | Deny | Does not want to keep development of merits—with/without visual allegation | 678 | 0.1 |
| 39 | Deny | DAA or failure to follow prescribed treatment—with/without visual allegationi | 55 | 0.0 |
| Data errorsj | 3,263 | 0.6 | ||
| Total | 530,178 | 100.0 | ||
| SOURCES: Frequency data was obtained from the 2010 SSA-831 file. Basis information was obtained from RAND'due south SSA Programme Information User's Manual (Panis and others 2000) and exchanges with disability experts at SSA. | ||||
| NOTES: Values may not sum to 100 because of rounding. CE = consultative examination; CE is also a Regulation Basis Code; | ||||
| a. Fiscal eligibility for DI or SSI is normally determined at the SSA field office before the claim is referred to the DDS. For that reason, most cases determined financially ineligible are non represented in the 831 information created by the DDS. | ||||
| b. SGA is an earnings threshold used to decide eligibility for both DI benefits and SSI payments. In calendar yr 2012, the SGA threshold was $ane,010 per month for the nonblind and $1,690 for the blind. Someone engaging in SGA is denied at the field function and non evaluated further. And, a DI beneficiary receives no benefits for whatever month in which he or she has earnings in a higher place the SGA threshold (with some exceptions for piece of work incentives). The SGA threshold is wage-indexed. | ||||
| c. No visual accusation means the applicant is not alleging blindness. | ||||
| d. Code 44 was initially used to indicate a ChampionshipXVI SGA deprival, only in the early 1990s it was redefined to indicate a nonsevere denial for SSI children. | ||||
| e. Duration denials tin can be invoked at step ii or step 3. The duration examination does not apply to SSI applicants who are statutorily bullheaded. | ||||
| f. Although the inability decision process for children includes a medical screen and a functional assessment as a single stride (step 3), for belittling purposes we hash out them separately as step 3a and step 3b. | ||||
| g. Code 43 has dual meanings. For SSI adults information technology indicates the applicant was determined to be able to perform some work in the national economy and was denied. | ||||
| h. Collateral estoppel: If there has been a prior favorable determination past SSA or the court, information technology must be adopted for the same menstruum on the new claim, with certain exceptions. | ||||
| i. Code 39 has the same meaning and employ for adult and child SSI applicants. It signifies denial for failure to follow prescribed treatment or, following a 1996 Congressional Human action, denial of applicants for whom DAA was found material to the finding of disability. | ||||
| j. Includes records with unknown RB (RBC = ZZ), RB not available (RBC = [blank]), obsolete codes, and other data errors. | ||||
Notes
1 Plan administrators differentiate "medical allowances" (based solely on the medical Listings) from "medical-vocational allowances" (which crave a severe harm, simply also accept into account residual functional capacity, historic period, past work, and education).
2 Plan administrators typically use "resource" to refer to financial assets such as savings or stocks. Administrators implement a limitation on financial assets, and they refer to it as the "resources test."
3 In 1999, SSA began the Prototype pilot in 10 states, whereby claims can be appealed direct to the administrative law judge level without going through the reconsideration phase.
4 In describing the disability determination procedure, "medical" is used in 2 means. First, it is used to distinguish the determination of medical eligibility using the v-footstep sequential process described in this annotation from the determination of financial eligibility, such as insured status (for DI) or income and resource eligibility (for SSI). Second, in discussing the five-step process, program administrators differentiate medical allowances (based solely on the medical Listings) from medical-vocational allowances (which require a severe harm, but also take into account residual functional capacity, age, past work, and education); run across note 1.
5 For instance, activities involving cocky-care, household tasks, unpaid grooming, hobbies, therapy, schoolhouse attendance, clubs, or social programs are not mostly considered to exist SGA. For more particular, run across the publicly available Program Operations Manual (POMS), https://secure.ssa.gov/apps10/poms.nsf/lnx/0410501001, or the Code of Federal Regulations (CFR), http://www.ecfr.gov/cgi-bin/retrieveECFR?gp=&SID=efc4db7ae17950f4db4ddfdf34e13c74&due north=20y2.0.1.i.5.sixteen&r=SUBPART&ty=HTML#20:two.0.1.1.5.sixteen.188.10.
vi Applicants are as well screened with respect to a host of other nonmedical requirements. For example, for TitleTwo dependent benefits, spouses and children must provide proof of their human relationship to the wage earner and, when applicative, their age. Survivors must provide decease certificates. Proof of citizenship or permanent residence is required according to statute. Proof that the claimant is non incarcerated may be required. In addition, TitleIi spousal benefits may require demonstration that the ex-spouse has not remarried. These and other nonmedical factors are checked by field offices, typically earlier the case is referred to the DDS.
7 Claims denied at the SSA field role level are non referred to the DDS agencies, and then 831 records are not typically created. Hence, for example, field role denials for insured condition, income test/resources test, incarceration, or noncitizenship are all considered technical denials, simply they are not represented in the RBC. A small pct of SGA denials may be included in the RBC—typically those remanded from the DDS to the field role. Researchers interested in field role determinations should admission the TitleIi Disability Research File or the Championship16 Disability Research File.
8 See the publicly available Program Operations Transmission, https://secure.ssa.gov/apps10/poms.nsf/lnx/0424505001.
9 For more than detail on the Listings, see the publicly available Program Operations Transmission, https://secure.ssa.gov/apps10/poms.nsf/subchapterlist!openview&restricttocategory=04340 or see http://world wide web.socialsecurity.gov/disability/professionals/bluebook/listing-impairments.htm.
ten In some cases, the analysis of past work can extend further than 15 years dorsum into the claimant's piece of work history. See https://secure.ssa.gov/apps10/poms.nsf/lnx/0425005015.
11 In certain cases, including mental impairments, the vocational grid is not used or information technology is used as a general framework. For more detail on the vocational grid, see the publicly available Plan Operations Manual, https://secure.ssa.gov/apps10/poms.nsf/subchapterlist!openview&restricttocategory=04250, or the Code of Federal Regulations, http://world wide web.ecfr.gov/cgi-bin/text-idx?c=ecfr&SID=ece928d7f4cda42f9d9a43f83b661174&rgn=div8&view=text&node=20:2.0.1.1.5.sixteen.194.35&idno=20.
12 See the Lawmaking of Federal Regulations, http://www.socialsecurity.gov/OP_Home/cfr20/404/404-1562.htm and http://www.socialsecurity.gov/OP_Home/cfr20/416/416-0962.htm.
13 Alabama, Alaska, office of California, Colorado, Louisiana, Michigan, Missouri, New Hampshire, New York, and Pennsylvania.
14 See the publicly bachelor Program Operations Transmission, https://secure.ssa.gov/apps10/poms.nsf/lnx/0425005005, the Code of Federal Regulations, http://www.ecfr.gov/cgi-bin/text-idx?c=ecfr&SID=ece928d7f4cda42f9d9a43f83b661174&rgn=div8&view=text&node=20:two.0.i.1.5.16.194.35&idno=20, and the Federal Register, Vol. 76, No. 177, Tuesday, September 13, 2011, http://world wide web.gpo.gov/fdsys/pkg/FR-2011-09-13/pdf/2011-23396.pdf. For implementation of expedited vocational cess in prototype states, run into http://www.socialsecurity.gov/disability/Documents/Prototype_Operating_Instructions.doc (p. 17).
15 However, children's insurance benefits under TitleII are bachelor for a child of a parent who is entitled to retirement or disability benefits or who is deceased. Generally, benefits are available after the age of xviii for a disability that began prior to that age. For more information, see https://secure.ssa.gov/poms.nsf/lnx/0410115001.
16 Although the inability determination process for children includes a medical screen and a functional assessment every bit a single footstep (step 3), for belittling purposes we discuss them separately as footstep 3a and step 3b.
17 The 3 recodes were quite consistent, though not identical. Nonetheless, the reasons for the slight differences fall into three categories. First, the coding for Lahiri, Vaughan, and Wixon (1995); Hu and others (2001); Dwyer and others (2002/2003); and Lahiri, Song, and Wixon (2008) was derived from an belittling sample of 831 records, and several very low-frequency code values that did not occur in the sample were not classified. Second, because of the nature of the tables used in the DI and SSI statistical reports (SSA 2011, 2011b), the recode did non include step 1 outcomes relating to fiscal eligibility determination, in contrast to the other studies. Tertiary, the belittling studies excluded children from their recodes, whereas the annual SSA publications include children.
18 The codes shown in Tables 1 through 3 are those used in the 831 files; other data sets that are derived from the NDDSS may apply RBCs that are not identical to those used in the 831 data. For example, the Disability Operational Information Store (DIODS), a data base constructed from the NDDSS system, uses a three-character variable for its TitleSixteen RBCsouth—a alphabetic character prefix, followed by the two-place numerical code used in the 831 information. Yet, the Disability Research File uses the same RBC found in the 831 information.
xix Note that the great recession may have affected both the number and limerick of determinations made in 2010.
References
Autor, David, Nicole Maestas, Kathleen Mullen, and Alexander Strand. 2011. "Does Delay Cause Disuse? The Effect of Administrative Determination Fourth dimension on the Labor Forcefulness Participation and Earnings of Disability Applicants." MRRC Working Paper No. 2011-258. Ann Arbor, MI: Academy of Michigan Retirement Inquiry Heart.
Ball, Robert M. 1978. Social Security: Today and Tomorrow. New York, NY: Columbia University Press.
Dwyer, Debra, Jianting Hu, Denton R. Vaughan, and Bernard Wixon. 2002/2003. "Counting the Disabled: Using Survey Self-Reports to Estimate Medical Eligibility for Social Security's Disability Programs." Journal of Economical and Social Measurement 28(three): 109–142.
Hu, Jianting, Kajal Lahiri, Denton R. Vaughan, and Bernard Wixon. 2001. "A Structural Model of Social Security's Disability Determination Process." The Review of Economic science and Statistics 83(two): 348–361.
Lahiri, Kajal, Jae Song, and Bernard Wixon. 2008. "A Model of Social Security Disability Insurance Using Matched SIPP/Administrative Data." Journal of Econometrics 145(1–two): four–20 (July).
Lahiri, Kajal, Denton R. Vaughan, and Bernard Wixon. 1995. "Modeling SSA's Sequential Disability Determination Process Using Matched SIPP Data." Social Security Bulletin 58(iv): 3–42.
Panis, Constantijn, Ronald Euller, Cynthia Grant, Melissa Bradley, Christin E. Peterson, Randall Hirscher, and Paul Steinberg. 2000. SSA Program Data User'southward Manual [RAND Manual]. Prepared by the RAND Corporation (contract no. PM-973-SSA) for the Social Security Administration.
[SSA] Social Security Administration. 2011a. Annual Statistical Report on the Social Security Disability Insurance Program, 2010. Washington, DC: Function of Retirement and Disability Policy, Office of Research, Evaluation, and Statistics.
———. 2011b. SSI Annual Statistical Study, 2010. Washington, DC: Office of Retirement and Disability Policy, Role of Research, Evaluation, and Statistics.
Source: https://www.ssa.gov/policy/docs/rsnotes/rsn2013-01.html
0 Response to "Disability Determination Decision Under Review Step 2 of 3"
Post a Comment